FY 2008 President's Budget Request for NIAAA - Director's Statement Before the Senate Subcommittee on Labor-HHS Appropriations
Statement by Ting-Kai Li, M.D., Director
National Institute on Alcohol Abuse and Alcoholism
National Institutes of Health
Department of Health and Human Services
March 26, 2007
Mr. Chairman and Members of the Committee, thank you for giving me the opportunity to update you on the activities of the National Institute on Alcohol Abuse and Alcoholism. I am Ting-Kai Li, Director of NIAAA, the lead agency for research on the health effects of alcohol. I am pleased to be here today with my distinguished colleagues from NINDS, NIMH, NIDA, and NIDCD to speak to the theme of Mind, Brain and Behavior. Those of us addressing you today have a fundamental mission – to reduce the substantial burden of illness caused by neurological and mental disorders, and by drug and alcohol abuse. Many of these disorders tend to manifest early in life, produce lifelong disability, derail individual potentials, and create tremendous burdens for families and significant cost to society. In fact, excessive alcohol use alone costs the United States an estimated $185 billion annually. [1] The FY 2008 budget for NIAAA includes $436,505,000.
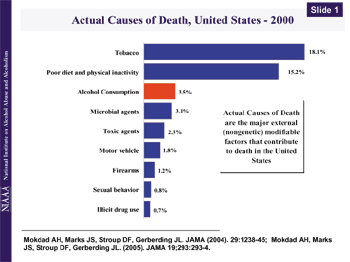
The HHS Centers for Disease Control and Prevention ranks alcohol as the third leading cause of preventable death in the United States (Figure 1), and the World Health Report ranks alcohol as the third leading risk factor for disease in developed countries. Although alcohol primarily targets two organs, the brain and liver, it has a wide range of effects throughout the body and NIAAA’s research portfolio encompasses all aspects of alcohol and health. In keeping with the theme of this Hearing, I will focus on the brain and behavior.
As illustrated in Figure 2, alcohol can negatively affect the body and brain at all stages of life resulting in a range of consequences, including consequences from maternal alcohol consumption on the developing embryo/fetus to alcoholic liver disease and dementia in later life. Throughout the lifespan, it is important to recognize the contribution of developmental stage, individual differences – both genetic and environmental, and dose and duration of alcohol exposure to potential outcomes. The substantially different effects and consequences of alcohol exposure at different stages of life necessitate different research strategies.

Today I would like to give you an overview of NIAAA’s progress in three areas to reduce the burden of illness due to alcohol. First, I will describe prevention efforts focused on early life stages. Second, I will describe new findings that can be used to improve the diagnosis and early detection of alcohol use disorders (AUDs). Finally, I will describe efforts to personalize medicine for those suffering from alcohol dependence.
PREVENTION
Prevention is a key focus of NIAAA, especially for pregnant women, children and adolescents. By altering harmful drinking behavior we can significantly reduce the burden of illness due to alcohol. Exposure of the developing embryo/fetus can result in alcohol-induced birth defects, t he most severe of which is fetal alcohol syndrome (FAS), a devastating developmental disorder that may include mental retardation. Individuals who do not exhibit the extent of symptoms characteristic of FAS may still have lifelong physical and/or neurological deficits as a result of in utero alcohol exposure. In addition, prenatal alcohol exposure itself may be a risk factor for subsequent alcohol dependence later in life. Therefore, NIAAA is supporting research to develop effective outreach to pregnant women, and approaches to intervene to protect against injury in the affected fetus and ameliorate deficits in the affected child.
Prevention in young children is also important, especially for those at high risk for early alcohol use. The period from birth to age 10 is a remarkable period of development, and although relatively few children in this age group are drinking alcohol, much is happening that will influence their path toward or away from early alcohol use. A number of the factors that put children at risk for early alcohol use are common to a wide range of adverse behavioral outcomes such as delinquency and other substance use. Even as young as preschool age, such children often have difficulties with impulse control and exhibit unusually high levels of aggression. NIAAA, NIMH, and NIDA are working to understand the personality/ temperament characteristics that predispose to early-onset mental and alcohol/ drug use disorders.
It is also essential to prevent and reduce underage alcohol use. Analyses of NIAAA’s National Epidemiologic Survey on Alcohol-Related Conditions ( NESARC) showed that 40% of individuals who reported drinking before the age of 15 also described their drinking behavior in a way consistent with a diagnosis of alcohol dependence. In fact, the highest prevalence of alcohol dependence in the United States occurs in the 18-24 year old age group. In addition, binge-drinking (i.e. drinking five or more drinks per occasion), which is popular with today’s young people, results in acute consequences such as traffic fatalities, alcohol poisoning, suicides, homicides and drownings. Non-fatal, but potentially life altering consequences such as sexual assault and violence also result. As part of a larger effort focused on underage drinking research, NIAAA provided the scientific foundation for the Surgeon General’s Call to Action to Prevent and Reduce Underage Drinking and continues to inform the work of the Interagency Coordinating Committee on the Prevention of Underage Drinking.
Recognizing that the brain continues to develop throughout adolescence and into early adulthood, NIAAA is investing in research to determine the short and long-term effects of alcohol on the developing brain and the degree to which it can recover from these insults. Such studies, including one in collaboration with NIMH intramural scientists, may identify changes in brain wiring that are associated with dependence or affect cognitive functioning. In addition, given the difference in patterns of alcohol use between boys and girls as they move through adolescence, NIAAA is investigating the interplay of hormones, brain development and alcohol use.
DIAGNOSIS
It is important to identify individuals who are at risk for adverse alcohol-related health outcomes because of their drinking behavior. Excessive alcohol intake over time leads to cumulative organ damage, especially alcoholic liver disease and increased risk of coronary artery disease, stroke and dementia. Early diagnosis of harmful drinking would enable health care providers to intervene to prevent a range of adverse health outcomes.
As shown in Figure 3, diagnostic criteria for Alcohol Abuse currently rely on an individual experiencing one or more alcohol-related problems associated with either the social or legal system, such as being cited for Driving While Intoxicated or problems with a spouse or family member. Diagnosis of Alcohol Dependence requires meeting three of seven criteria relating to physiological changes such as the development of tolerance to increased amounts of alcohol or the experience of withdrawal symptoms, behavioral maladaption characterized by loss of control and compulsion to drink, and negative consequences from this drinking pattern. This categorical approach does not favor early diagnosis and intervention.
Today I report recent findings from analyses of NESARC that will improve the diagnosis of alcohol dependence. Further, alcohol abuse and dependence have long been treated as independent disorders. New findings indicate that they represent a continuum of severity of alcohol use problems. The analyses suggest we may be able to use questions that reveal an individual’s pattern of drinking to identify the risk of developing AUDs. In much the same way that numerical measurements of blood pressure,
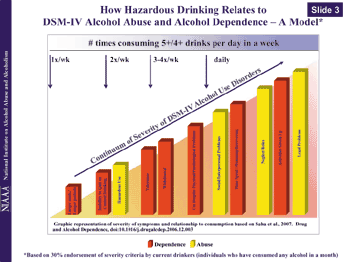
cholesterol and triglycerides relate to relative risk for cardiovascular disease, the best indicators of developing alcohol problems are measures of how frequently an individual engages in a harmful pattern of drinking. Specifically, recent findings relate data on the frequency of binge drinking and the maximum number of drinks consumed to risk for organ damage and to alcohol dependence. Through clinical studies, we may be able to determine appropriate cut points to define AUDs and also to gauge one’s risk of developing alcohol problems. Just as physicians treat high cholesterol before an individual experiences a heart attack, they will be able to intervene before an individual loses control of drinking. Diagnosis centered on harmful drinking patterns should also help health care providers differentiate between alcohol related neurocognitive deficits in the elderly and Alzheimer related dementia.
MEDICATIONS DEVELOPMENT
NIAAA is supporting research on a number of fronts to improve treatment options for alcohol dependence. Studies in animal models focusing on signaling pathways in the brain have produced additional targets for human studies. For example, the anxiety that people with alcohol dependence experience when they stop drinking is a powerful motivator for them to resume. In addition, stress can trigger relapse to heavy drinking after a period of abstinence. Therefore, medications are being tested that target molecules involved in biological pathways that mediate stress and anxiety such as corticotrophin-releasing factor, neuropeptide Y, and nociceptin receptors. Also being tested are medications that target the metabolism of endocannabinoids, naturally occurring substances in the brain that act on the same receptors as the active ingredients of marijuana and have been shown to play a role in regulating appetite for alcohol.
TREATMENT RESEARCH
In addition to developing new medications and determining the genetic and environmental factors that contribute to the initiation and escalation of drinking, it is equally important to understand how individuals change harmful drinking patterns. The majority of young adults change harmful drinking behaviors without treatment. Adults seek treatment when alcohol dependence becomes chronic and relapsing, generally in the period of midlife. Data from clinical trials raise the question of whether treatment itself is responsible for the improvement in drinking behavior or if the positive motivation to seek treatment actually underlies a substantial part of the treatment success. Further, evidence has shown that a wide array of available therapeutic approaches yields similar results, suggesting that it is not the particular technique that is responsible for change but other common underlying factors. As a result, NIAAA is focusing on addressing underlying mechanisms of change across all behavioral treatments, identifying the factors that contribute to behavioral change and lead to sustained recovery. This research will improve clinical practice both by identifying key aspects of therapy that must be present for maximum effectiveness and by facilitating the delivery of more finely tuned individualized treatment. We also need to be particularly mindful of health disparities. A recent study suggests that Hispanics and Blacks with higher levels of problem severity were less likely to have used treatment services than Whites with problems of comparable severity.
Taken together, these strategies of improved prevention, better diagnosis and personalized treatment are expected to reduce the burden of alcohol-related illnesses over the long term and lead to better health outcomes for the nearly 18 million American adults who, in any year, struggle with alcohol use disorders [2] .
Ting-Kai Li, M.D., Director, National Institute on Alcohol Abuse and Alcoholism, National Institutes of Health, Department of Health and Human Services
Dr. Ting-Kai (T. K.) Li was appointed to the position of the Director of the National Institute on Alcohol Abuse and Alcoholism (NIAAA) in November 2002. The NIAAA is a component of the National Institutes of Health (NIH) within the U.S. Department of Health and Human Services.
Throughout his distinguished research career, Dr. Li has been at the center of advances that have transformed both the way alcoholism is understood and the means of investigating alcohol's effects on the body and brain. A major focus of Dr. Li's research has been to characterize the structure and dynamics of the multiple genetic variants of alcohol dehydrogenase (ADH), the enzyme that catalyzes the first step in the metabolism of ethanol and the differences among individuals in the physiology of these enzymes. Dr. Li also pioneered the development of animal models in which marked differences in the level of voluntary alcohol consumption could be observed, paralleling the same inborn variation seen in human behavior. The development of these animal lines helped cement the once radical notion that alcohol consumption behavior was genetically influenced.
Born in Nanjing, China, Dr. Li earned his undergraduate degree from NorthwesternUniversity, his M.D. from HarvardUniversity, and completed his residency training at PeterBentBrighamHospital in Boston, where he was named chief medical resident in 1965. He also conducted research at the Nobel Medical Research and Karolinska Institutes in Stockholm and served as deputy director of the department of biochemistry within the Walter Reed Army Institute of Research. Dr. Li joined the faculty at IndianaUniversity as professor of medicine and biochemistry in 1971. He subsequently was named the school's John B. Hickam Professor of Medicine and Professor of Biochemistry and later Distinguished Professor of Medicine. In 1985 he became director of the Indiana Alcohol Research Center (IARC) at the Indiana University School of Medicine, where he also was the Associate Dean for Research.
Dr. Li is the author of more than 400 journal articles and book chapters, has been invited to deliver many major lectureships in countries across the world, and is the recipient of numerous prestigious awards for his scientific accomplishments, including the Jellinek Award, the James B. Isaacson Award for Research in Chemical Dependency Diseases, and the R. Brinkley Smithers Distinguished Science Award.
Dr. Li has also served in many prominent leadership and advisory positions, including past President of the Research Society on Alcoholism (RSA), and as a member of the National Advisory Council on Alcohol Abuse and Alcoholism and the Advisory Committee to the Director, NIH. Dr. Li was elected to membership in the Institute of Medicine of the National Academy of Sciences in 1999 and is also an honorary fellow of the United Kingdom's Society for the Study of Addiction.
Department of Health and Human Services
Office of Budget
Richard J. Turman
Mr. Turman is the Deputy Assistant Secretary for Budget, HHS. He joined federal service as a Presidential Management Intern in 1987 at the Office of Management and Budget, where he worked as a Budget Examiner and later as a Branch Chief. He has worked as a Legislative Assistant in the Senate, as the Director of Federal Relations for an association of research universities, and as the Associate Director for Budget of the National Institutes of Health. He received a Bachelor’s Degree from the University of California, Santa Cruz, and a Masters in Public Policy from the University of California, Berkeley.
[1] Harwood, H. Updating Estimates of the Economic Costs of Alcohol Abuse in the United States: Estimates, Update Methods and Data (2000) . https://pubs.niaaa.nih.gov/publications/economic-2000/
[2] Grant BF, Dawson DA , Stinson FS, Chou SP, Dufour MC, and Pickering RP. Drug and Alcohol Dependence 2004. 74: 223-234.
Updated: September 2009

