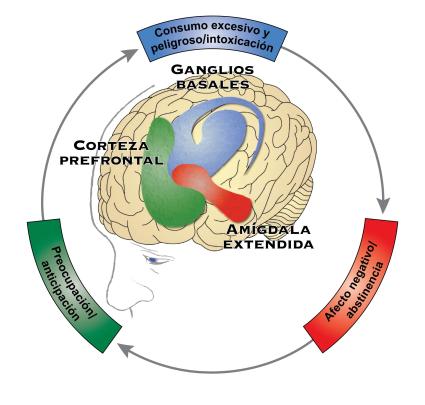
Goal 1: Elucidate the Biological Mechanisms and Consequences of Alcohol Misuse
NIAAA’s Long-Term Vision
To comprehensively understand the biological processes affected by alcohol misuse to inform the prevention, diagnosis, and treatment of alcohol-related problems.
Alcohol misuse has powerful effects on the brain and behavior. Neuroscience research has characterized the short-term impact of alcohol on brain activity and the adaptations in brain structure and function that occur as individuals progress from occasional, controlled alcohol use to alcohol misuse and alcohol use disorder (AUD). This work has made major strides in shedding light on the neurotransmitter systems and neurobiological mechanisms that are altered by alcohol and that contribute to the development of alcohol misuse and AUD. Equally important, neuroscience advances are laying the foundation for understanding the individual differences that drive alcohol misuse across the life span. Innovative research to elucidate the biological mechanisms of alcohol-associated pathology and recovery within a neurobiological framework can reveal novel opportunities for more effective prevention, diagnosis, and treatment of alcohol misuse and AUD.
Alcohol misuse also has powerful effects beyond the brain and can damage nearly every organ system in the human body. While the liver is the primary site of alcohol metabolism and is susceptible to alcohol-associated injury and disease, alcohol misuse is a significant contributor to pancreatitis, cardiovascular disease, cancer, and other health conditions. Additionally, alcohol misuse can negatively impact the complex interactions between organ systems. For example, research demonstrates that alcohol-related neurobiological changes may not be due entirely to the direct actions of alcohol on the brain but may be mediated partially through interactions with the gastrointestinal tract, liver, and endocrine system. Basic, translational, and clinical research is needed to better characterize the mechanisms through which alcohol misuse damages the body’s organ systems and leads to, and exacerbates, chronic disease.
Additionally, understanding the biological mechanisms underlying the effects of prenatal alcohol exposure, from prenatal development to adulthood, and understanding other medical challenges, such as HIV/AIDS, can inform preventive, diagnostic, and therapeutic strategies to improve health outcomes. See the Fetal Alcohol Spectrum Disorders and Alcohol and HIV discussions within the Cross-Cutting Research Programs section for more information on these specific research areas.
Goal 1 research topics are integrally linked to the Cross-Cutting Research Themes. Examples of NIAAA research priorities in this area include the following objectives.